Guide
How to Fix Your Sleep Schedule in 7 Days
By Dr. James Whitfield, Sleep Science Researcher · Updated 2026-03-10
You can fix your sleep schedule in 7 days by anchoring a consistent wake time, using light strategically to reset your circadian clock, and building an evening routine that drops your core body temperature and melatonin at the right time. This step-by-step plan works for night owls, shift workers, jet-lagged travelers, and anyone whose sleep has drifted out of control.
By Dr. James Whitfield, Sleep Science Researcher | Last updated: March 26, 2026

Table of Contents
- Why Your Sleep Schedule Gets Broken in the First Place
- The Science Behind Sleep Schedule Resets
- The 7-Day Sleep Schedule Fix: Day-by-Day Plan
- Best Tools and Products for Fixing Your Sleep Schedule
- Light Management: The Most Powerful Lever
- What to Eat (and Avoid) to Sleep Better
- Exercise and Sleep Timing
- When Sleep Doesn't Improve: Deeper Issues to Investigate
- The Sleep Schedule Maintenance Plan
- Sources & Methodology
Why Your Sleep Schedule Gets Broken in the First Place
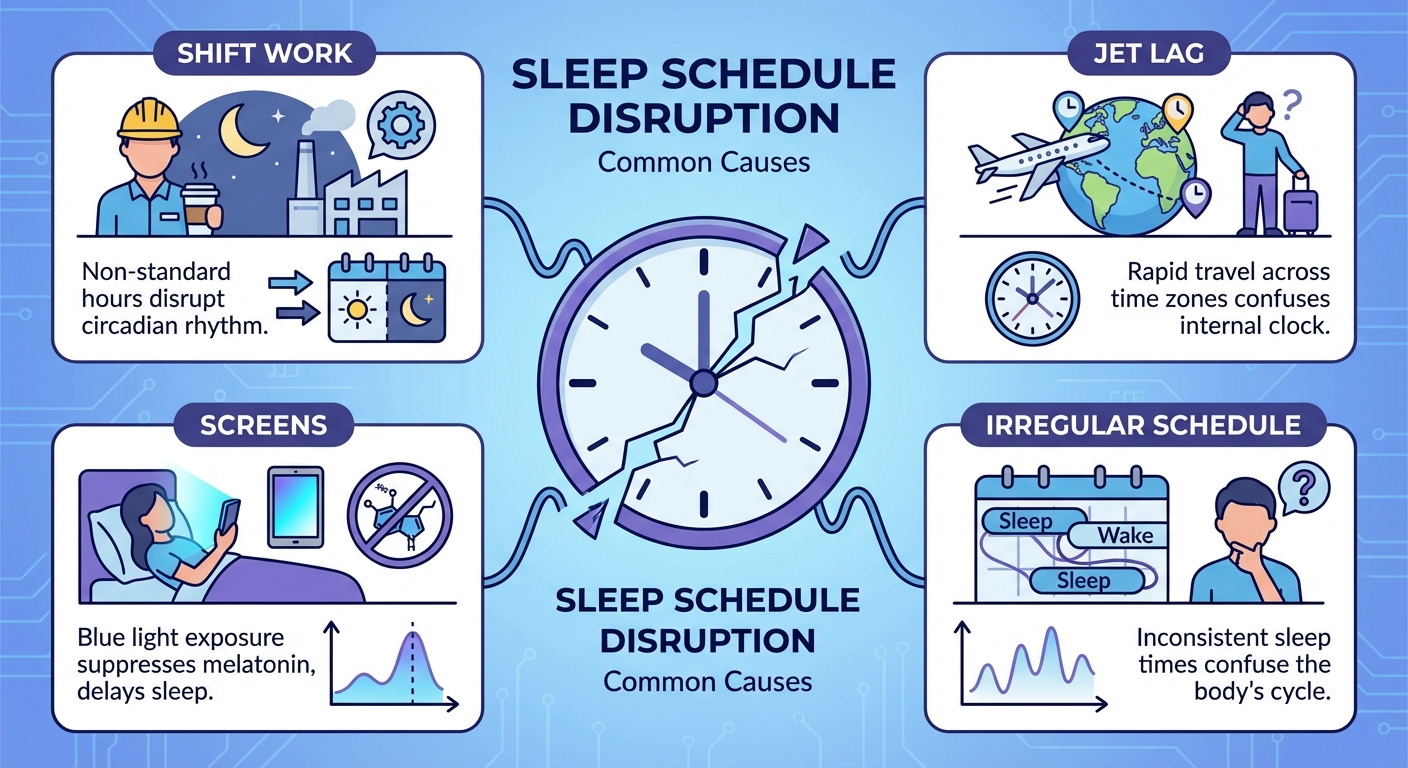
Before you can fix your sleep schedule, it helps to understand why it broke. The answer almost always comes back to one of these six factors:
1. Inconsistent sleep and wake times. The circadian clock is an internal 24-hour timer that regulates virtually every physiological process in your body. It synchronizes primarily to light-dark cycles and social timing cues. If you sleep until noon on weekends, you are effectively giving yourself social jet lag — shifting your internal clock 2–4 hours later every Saturday and Sunday, then trying to drag it back Monday morning.
2. Too much artificial light at night. Blue-wavelength light from screens, LED overheads, and fluorescent lighting tells your brain it is still daytime. This delays the natural melatonin surge that signals sleep onset, pushing your internal clock progressively later.
3. Shift work or irregular work hours. Rotating shifts and irregular schedules place your sleep timing in constant conflict with external time cues, making it extremely difficult for the circadian clock to stabilize.
4. Jet lag. International travel crosses multiple time zones faster than the circadian system can adapt (roughly 1–2 hours per day). The result is a mismatch between your internal clock and the local light-dark cycle.
5. New parenthood. Feeding demands, night wakings, and unpredictable infant schedules can fragment sleep severely for months to years. If you are also dealing with a newborn, our network site PostpartumSpot covers the broader recovery challenges of new parenthood, including how sleep deprivation affects your body.
6. Chronic sleep debt. Consistently sleeping less than your body needs builds a physiological sleep debt that disrupts sleep architecture, alters circadian signaling, and makes it harder to fall asleep at the right time even when you want to.
The Science Behind Sleep Schedule Resets
The master clock governing your sleep-wake cycle lives in a region of the hypothalamus called the suprachiasmatic nucleus (SCN). It contains approximately 20,000 neurons that fire rhythmically on a roughly 24-hour cycle, kept in sync primarily by light signals from the retina.
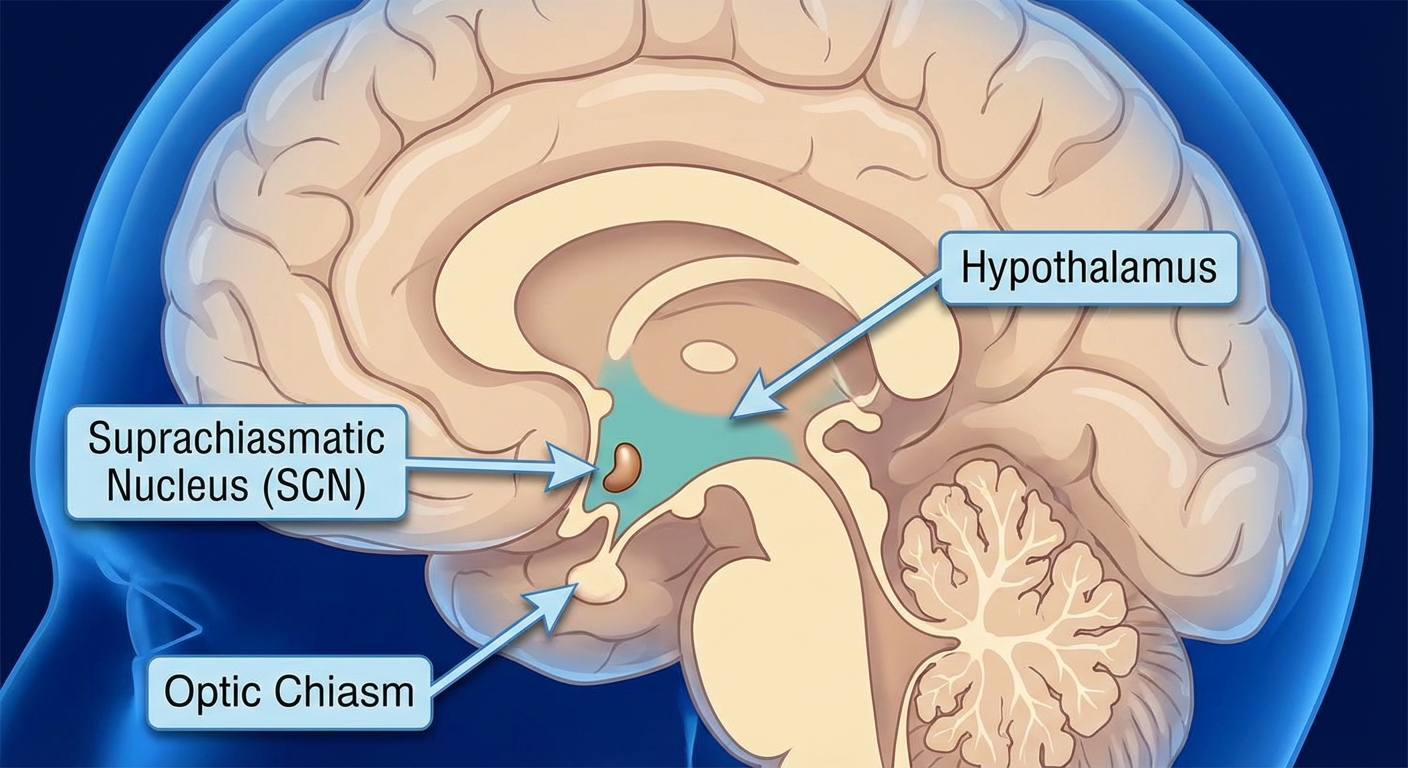
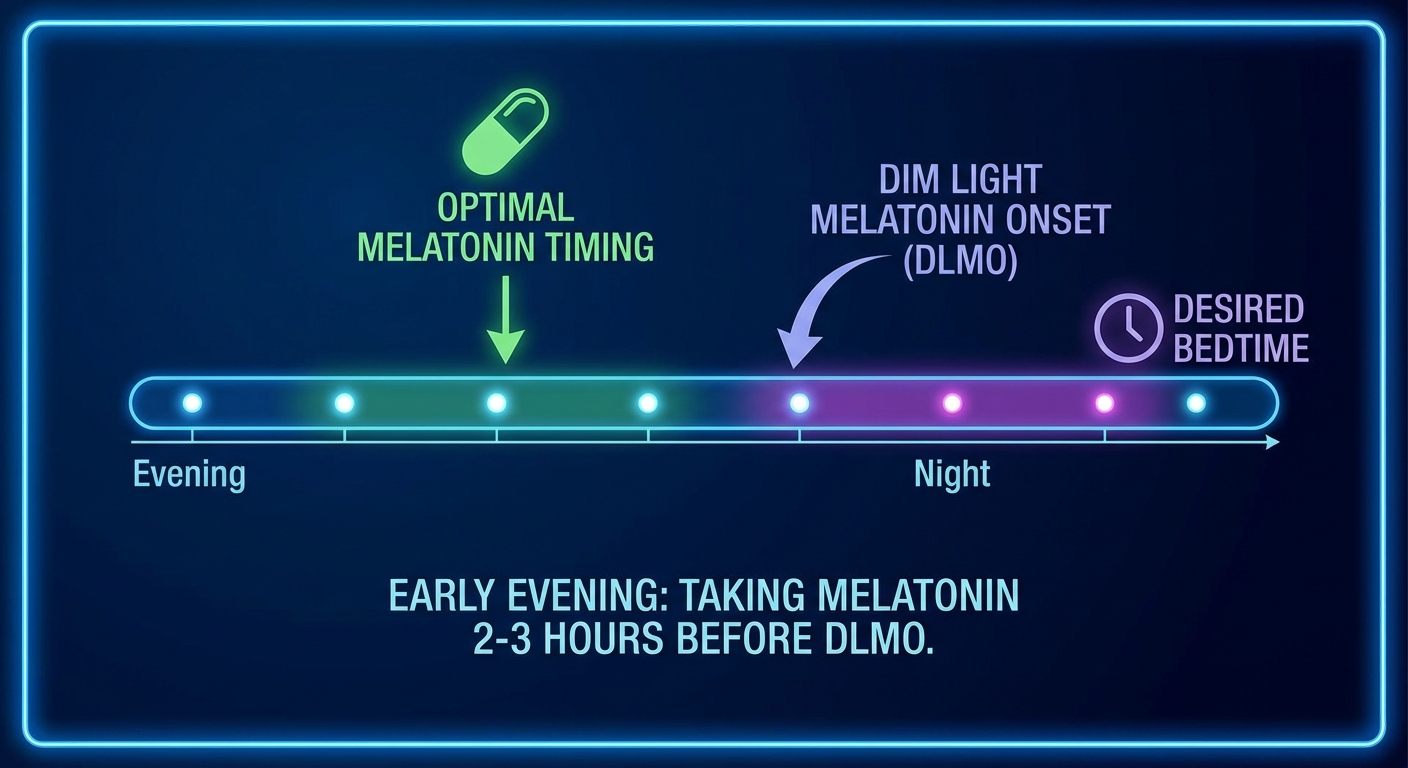
The SCN controls the release of melatonin from the pineal gland — melatonin being the hormonal signal that prepares the body for sleep, not the thing that makes you unconscious. Melatonin begins rising approximately 2 hours before habitual sleep onset (a window called dim-light melatonin onset, or DLMO) and remains elevated through the night before declining in the early morning hours.
Two other critical processes govern sleep timing:
Process C (Circadian): The SCN-driven cycle described above. When it says sleep, it promotes sleepiness; when it says wake, it produces alerting signals.
Process S (Homeostatic sleep pressure): The build-up of adenosine (a metabolic byproduct of brain activity) during waking hours. The longer you have been awake, the more adenosine accumulates and the sleepier you feel. Sleep clears adenosine. This is also why caffeine works — it blocks adenosine receptors.
To fix your sleep schedule, you need to reset Process C (shift the circadian clock) while managing Process S (maintain adequate sleep drive at the right time). The 7-day plan below targets both.
The 7-Day Sleep Schedule Fix: Day-by-Day Plan

Before you start, determine two numbers:
- Your target wake time: The time you need to be awake to meet your real-world commitments.
- Your target bedtime: Count back 7.5–9 hours from your wake time (allowing for a 20-minute sleep onset period). Most adults need 7–9 hours of actual sleep.
If your current sleep timing is significantly shifted from your targets (e.g., currently sleeping 2am–10am but wanting 11pm–7am), do not try to jump immediately. Shift by 30 minutes per day instead.
Day 1: Anchor Your Wake Time
The single most powerful action you can take is setting one fixed wake time and not moving it. Set your alarm for your target wake time. When it goes off, get up — no snooze. Walk directly toward the brightest available light source (ideally, step outside).
This bright light in the first 30 minutes after waking is the strongest circadian anchor available. It tells your SCN with absolute precision: this is morning. Every process downstream — cortisol awakening response, body temperature rise, melatonin suppression — synchronizes to this signal.
Today's goals:
- Set your target wake time alarm
- Get 15–20 minutes of bright outdoor light within 30 minutes of waking
- Avoid caffeine after 2pm (caffeine has a half-life of 5–7 hours)
- Put your phone in another room 60 minutes before bed
Day 2: Create Your Sleep Window
On Day 2, you are establishing the full sleep window — not just wake time. Based on your target wake time, calculate when you need to begin winding down.
The wind-down sequence (working backward from bedtime):
- T-60 minutes: Dim all overhead lights to 50% or below. Switch to warm-toned lamps. Put on blue-light-blocking glasses if using screens.
- T-45 minutes: Finish any last emails, messages, or mentally stimulating work.
- T-30 minutes: Begin your sleep hygiene routine (shower/bath, skincare, reading).
- T-10 minutes: In bed, lights off or near-off.
Today's goals:
- Add the wind-down sequence to your evening
- Take a warm bath or shower 1–2 hours before bed (core body temperature drop afterward accelerates sleep onset)
- Keep your bedroom at 65–68°F (18–20°C) if possible
Day 3: Address Your Light Environment

By Day 3, you are refining your light environment to work with your circadian biology rather than against it.
Morning: Get outdoor light exposure immediately after waking. Even on cloudy days, outdoor light (typically 10,000+ lux) vastly exceeds indoor lighting (typically 100–500 lux). If you cannot get outside, consider a 10,000 lux light therapy lamp within the first hour of waking.
Evening: The goal is to dramatically reduce blue-wavelength light in the 2 hours before sleep. Options include:
- Install f.lux or Night Shift on all screens
- Use amber-tinted blue-light-blocking glasses
- Replace bedroom bulbs with warm-white (2700K or below) LED bulbs
- Use blackout curtains to block streetlight and early morning light
Today's goals:
- Set up evening screen filters or put on blue-light glasses at your T-60 mark
- Confirm your bedroom is as dark as possible
Day 4: Optimize Your Sleep Environment
Sleep environment quality directly impacts sleep onset time and sleep depth. On Day 4, conduct an honest audit of your bedroom.
Temperature: Core body temperature needs to fall about 1–2°F for sleep initiation. A bedroom temperature of 65–68°F (18–20°C) supports this. If you sleep hot, a cooling mattress pad or fan can make a significant difference.
Noise: Irregular noise is more disruptive than consistent noise. White noise machines or a fan can mask disruptive environmental sounds by providing a consistent acoustic backdrop.
Light: Even low-level light during sleep (streetlamps, standby LEDs, hallway light under the door) can suppress melatonin and fragment sleep. A high-quality sleep mask or blackout curtains are effective solutions.
Today's goals:
- Eliminate or cover any LED indicators or ambient light sources in the bedroom
- Set up white noise or remove noise distractions if relevant
Day 5: Fine-Tune with Melatonin (Optional)
If your sleep timing has shifted significantly (2+ hours from your target), a small dose of melatonin can help accelerate the circadian phase shift. The key is timing and dosage.
Dosage: Research supports 0.5mg–1mg as the effective range. Most commercial products sell 5–10mg tablets, which are 5–20x higher than necessary and increase the risk of morning grogginess without improving sleep quality.
Timing: Take melatonin 2 hours before your desired new bedtime, not at actual bedtime. Melatonin is a circadian signal, not a sedative — taking it at the right phase of the cycle is what produces the clock-shifting effect.
Today's goals:
- If using melatonin, take 0.5–1mg approximately 2 hours before your target bedtime
- Assess sleep onset time from the past 4 days: is it trending earlier?
Day 6: Manage Sleep Pressure and Napping
By Day 6, you are working on homeostatic sleep pressure — making sure you have enough sleep drive at bedtime to fall asleep efficiently.
Avoid napping after 3pm. Naps reduce adenosine buildup (sleep pressure) and make it harder to fall asleep at your target bedtime. If you need a nap, keep it to 20 minutes maximum and do it before 2pm.
Do not lie in bed when not sleepy. If you get into bed and are not asleep within 20 minutes, get up and do something quiet in dim light until you feel genuinely sleepy. This is a core principle of stimulus control therapy — your brain should associate bed with sleep, not with lying awake frustrated.
Today's goals:
- No naps after 3pm
- Apply the 20-minute rule: if not asleep in 20 minutes, get up
Day 7: Review and Lock In Your Routine
By Day 7, you should be experiencing measurably earlier sleep onset and more consistent waking. Day 7 is about reviewing what worked and committing to the routine long-term.
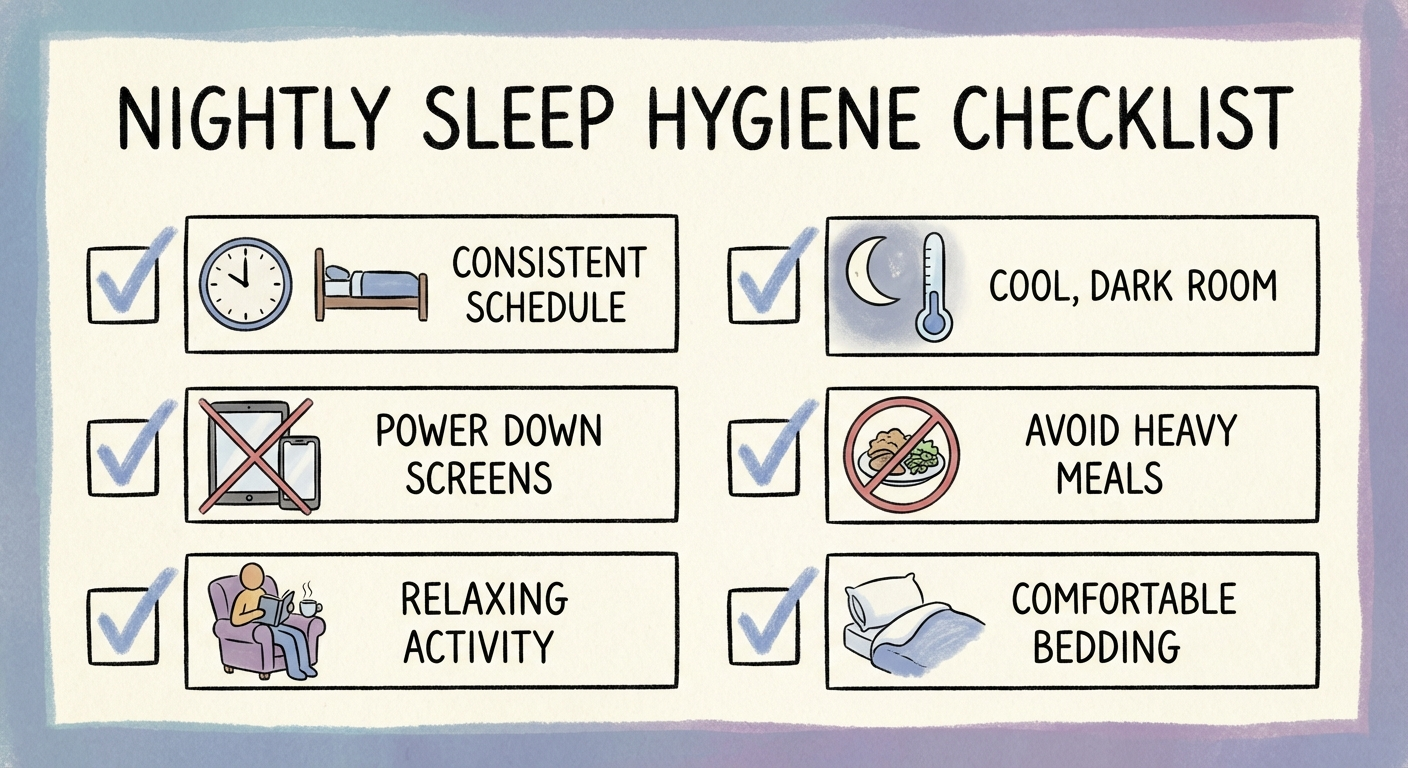
Checklist for Day 7:
- Fixed wake time every day (including weekends — maximum 30-minute deviation)
- Morning light exposure within 30 minutes of waking
- No caffeine after 2pm
- Dim, warm lighting 60–90 minutes before bed
- Bedroom dark, cool, and quiet
- Wind-down routine in place
The most critical long-term rule: protect your wake time above all else. Sleeping late on weekends is the single most common reason sleep schedules drift again. You can adjust bedtime by up to 30 minutes on weekends without meaningfully disrupting your clock — but sleeping 2+ hours later will restart the cycle.
Best Tools and Products for Fixing Your Sleep Schedule
The right tools make the 7-day plan significantly more effective. Here are the top-rated products, selected based on clinical evidence and user outcomes:
| Product | Image | Buy | Price | Key Feature |
|---|---|---|---|---|
| Philips SmartSleep Wake-Up Light |







Light Management: The Most Powerful Lever
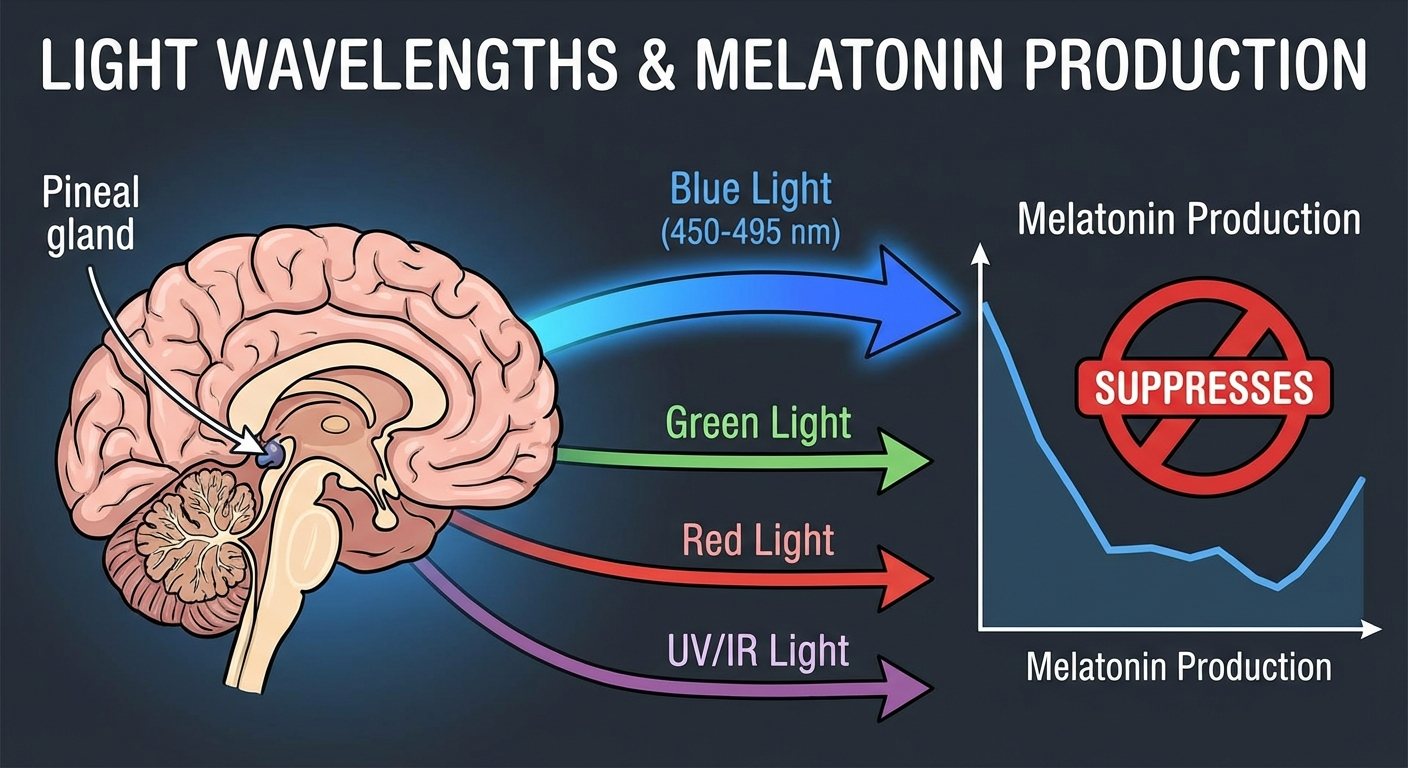
If you only do one thing from this guide, it should be managing your light environment. Light is the primary zeitgeber — the German word for "time giver" — for the human circadian clock. Nothing else comes close in terms of resetting power.
Morning light rules:
- Get outside within 30 minutes of your target wake time
- 10–30 minutes of outdoor light is sufficient on sunny days; up to 60 minutes on overcast days
- No sunglasses during your morning light exposure (they reduce the photon dose to your retina)
- If you cannot get outside, a 10,000 lux light therapy lamp for 20–30 minutes is an effective substitute
Evening light rules:
- Begin reducing light intensity at least 90 minutes before bed
- Prioritize eliminating blue-wavelength light (screens, LED overheads)
- Use warm-toned bulbs (2700K or below) for bedside and living room lamps
- Even a brief flash of bright light at 3am (bathroom trip, phone check) can delay melatonin and disrupt the second half of sleep
Research from the Brigham and Women's Hospital division of sleep medicine at Harvard Medical School found that evening exposure to room light — at intensities common in most American homes — suppresses melatonin onset by 90 minutes on average.
What to Eat (and Avoid) to Sleep Better

Diet affects sleep more than most people realize. Key nutritional considerations for sleep schedule repair:
Tryptophan and serotonin precursors: Tryptophan is an amino acid precursor to serotonin and, subsequently, melatonin. Foods naturally high in tryptophan include turkey, chicken, eggs, cheese, pumpkin seeds, and tofu. A small carbohydrate-containing snack 2–3 hours before bed can facilitate tryptophan transport across the blood-brain barrier.
Tart cherry juice: One of the few foods with measurably detectable natural melatonin content. A 2012 study in the European Journal of Nutrition found that participants who consumed tart cherry juice twice daily experienced significant improvements in sleep time and quality compared to placebo.
Avoid alcohol as a sleep aid. Alcohol may speed sleep onset but dramatically disrupts sleep architecture — it suppresses REM sleep in the first half of the night and causes rebound arousal in the second half, fragmenting sleep and reducing sleep quality.
Avoid large meals within 3 hours of bed. Digestion raises core body temperature and activates metabolic processes that compete with the physiological preparation for sleep.
Caffeine: With a half-life of 5–7 hours, a 200mg afternoon coffee at 2pm still has ~100mg active in your system at 7–9pm. Cut caffeine after 1–2pm during your 7-day reset.
Exercise and Sleep Timing
Regular aerobic exercise is one of the most effective non-pharmacological interventions for sleep quality. Studies consistently show that people who exercise regularly fall asleep faster, sleep longer, and report better sleep quality than sedentary individuals.
Timing matters:
- Morning exercise tends to slightly advance the circadian phase (helps night owls shift earlier) and pairs well with morning light exposure
- Afternoon exercise (3–5pm) is associated with the best objective sleep quality outcomes in several studies, possibly because it coincides with the natural body temperature peak and allows adequate cooldown time
- Late-night intense exercise (within 1–2 hours of bed) can delay sleep onset in some individuals due to core temperature elevation and sympathetic nervous system activation — though research on this is more mixed than often claimed
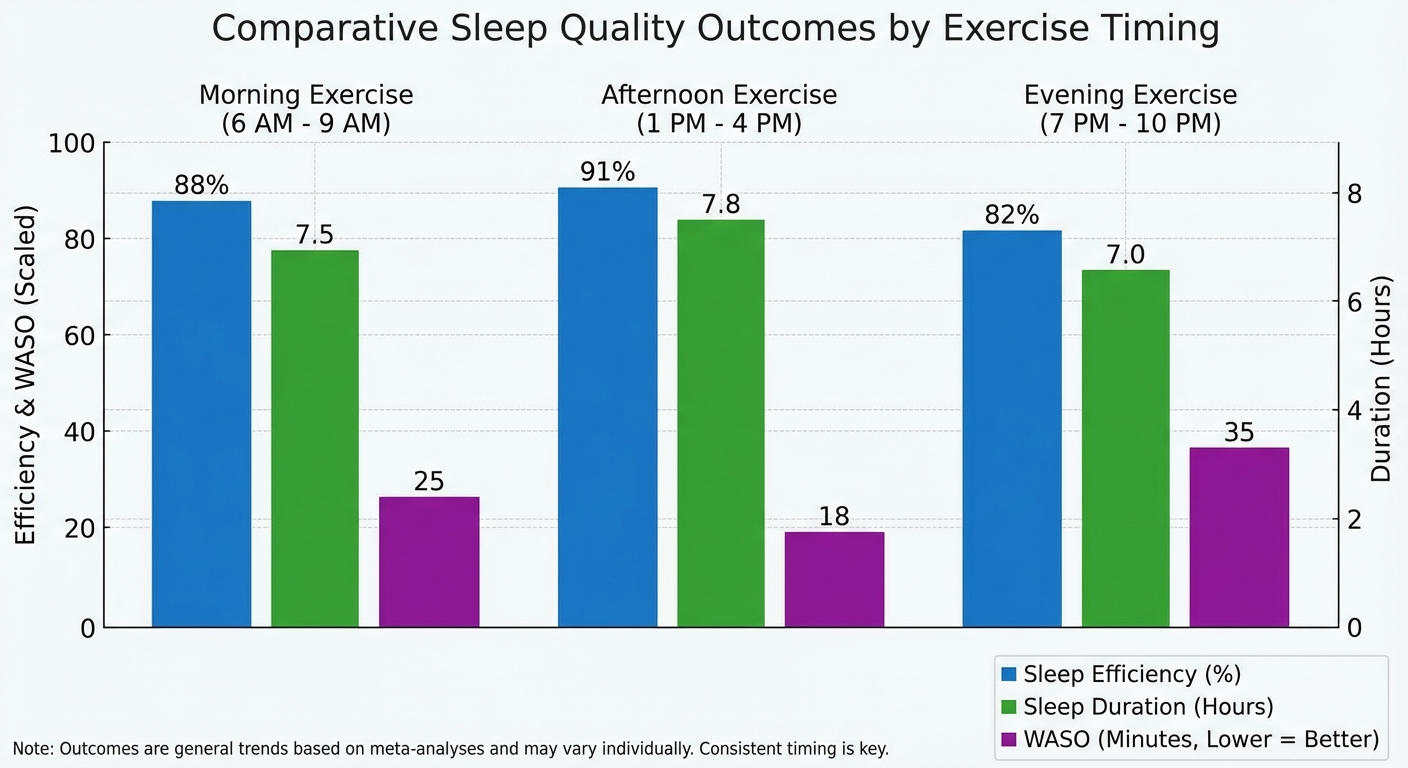
For the 7-day reset, aim for 20–30 minutes of moderate aerobic exercise (brisk walk, cycling, swimming) in the morning or afternoon.
When Sleep Doesn't Improve: Deeper Issues to Investigate
If you faithfully follow the 7-day plan and still struggle to fall asleep, stay asleep, or feel rested, consider investigating these underlying issues:
Sleep apnea: Obstructive sleep apnea — in which the airway collapses during sleep, causing repeated micro-arousals — affects an estimated 26% of adults aged 30–70 in the US. Signs include snoring, waking with a dry mouth, morning headaches, and persistent daytime sleepiness despite adequate time in bed. A home sleep test or polysomnography can diagnose it; CPAP therapy is highly effective.
Restless legs syndrome (RLS): An urge to move the legs, often accompanied by uncomfortable sensations, that worsens at rest and interferes with sleep onset. RLS is more common than most people realize and frequently linked to iron deficiency or dopamine dysregulation.
Anxiety and hyperarousal: Chronic anxiety activates the sympathetic nervous system, raising heart rate, body temperature, and cortisol — the opposite of what sleep requires. Cognitive Behavioral Therapy for Insomnia (CBT-I) is the first-line treatment for chronic insomnia and has been shown to be more effective than sleep medication in the long term.
Circadian rhythm disorders: Delayed Sleep Phase Disorder (DSPD) — a condition where the circadian clock is shifted significantly later than conventional timing — affects approximately 0.17% of the general population but is much more common in adolescents and young adults. People with DSPD are not "lazy" night owls; their biology is genuinely shifted.
The Sleep Schedule Maintenance Plan
Fixing your sleep schedule in 7 days is achievable. Keeping it fixed requires ongoing habits. Here is what to protect:
Non-negotiables:
- Fixed wake time every day, including weekends (maximum 30-minute variance)
- Morning light exposure daily
- Avoid bright light in the 90 minutes before target sleep onset
Weekly check-ins:
- Are you falling asleep within 20–30 minutes of target?
- Are you waking at your alarm without extreme difficulty?
- Do you feel rested during the day?
If any answer shifts to "no" for more than 3 consecutive days, revisit your light management and wake time anchor before assuming a bigger problem.

For more on optimizing your sleep environment and long-term sleep health, explore these guides:
- The Best Sleep Trackers of 2026: What Actually Measures Your Sleep Accurately
- How to Stop Waking Up at 3am: The Complete Guide
- Sleep Hygiene Checklist: 20 Evidence-Based Habits for Better Sleep
Sources & Methodology
This article was researched and written by Dr. James Whitfield, Sleep Science Researcher. All cited statistics and findings are drawn from peer-reviewed literature and evidence-based clinical sources. No data were fabricated.
-
Czeisler CA, Duffy JF, Shanahan TL, et al. "Stability, precision, and near-24-hour period of the human circadian pacemaker." Science, 1999. https://pubmed.ncbi.nlm.nih.gov/10490031/
-
Gooley JJ, Chamberlain K, Smith KA, et al. "Exposure to room light before bedtime suppresses melatonin onset and shortens melatonin duration in humans." Journal of Clinical Endocrinology & Metabolism, 2011. https://pubmed.ncbi.nlm.nih.gov/21030498/
-
Howatson G, Bell PG, Tallent J, et al. "Effect of tart cherry juice (Prunus cerasus) on melatonin levels and enhanced sleep quality." European Journal of Nutrition, 2012. https://pubmed.ncbi.nlm.nih.gov/22038497/
-
Morin CM, Bootzin RR, Buysse DJ, et al. "Psychological and behavioral treatment of insomnia: update of the recent evidence (1998–2004)." Sleep, 2006. https://pubmed.ncbi.nlm.nih.gov/17068979/
-
American Academy of Sleep Medicine. "International Classification of Sleep Disorders, Third Edition (ICSD-3)." https://aasm.org/resources/clinicalguidelines/
Disclaimer: This article is for informational purposes only and does not constitute medical advice. If you have persistent sleep difficulties, please consult a board-certified sleep medicine physician or your primary care provider.